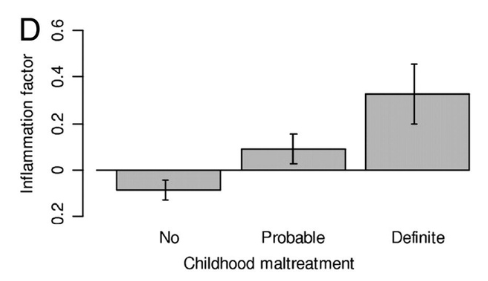
Although these adaptations can be helpful to reduce threats, they may lead over time to maladaptive outcomes including mental health problems. For example, inflammation levels are higher in individuals who have experienced maltreatment compared to those who haven’t, and are associated with mental health problems later on.

IoPPN researchers find lonely secondary school students less likely to gain employment in adulthood

New research from the Institute of Psychiatry, Psychology & Neuroscience (IoPPN) at King’s College London, in partnership with the University of Greenwich, has found that there is a direct socioeconomic impact of loneliness in early adolescence.
The research, published in Social Science and Medicine, found that lonely young adults are more likely to be out of education, employment, or training (NEET) and consider themselves less employable and lower on the economic ladder than their less lonely peers.
Sourcing data from the Environmental Risk (E-Risk) Longitudinal Twin Study, researchers followed the progress of 2,232 individuals born in England and Wales during 1994-1995. Participants were assessed at ages 12, 18 and 26 for levels of loneliness, as well as being asked to rate their social status. Participants’ employment status and employability were assessed at age 18.
Researchers found that young adults who had experienced loneliness earlier on in life experienced difficulties in young adulthood, even if they were no longer lonely. Researchers suggest that this demonstrates that loneliness impacts a person’s long term economic prospects and suggests that addressing loneliness in early adolescence could yield economic benefits through increased productivity.
“While there are clear impacts of loneliness on mental health from an early age, our study demonstrates that loneliness also negatively impacts a person’s employment prospects. We’ve shown that, from an early age, loneliness can have knock on effects on a person’s ability to compete in the job market. This not only harms a person’s chances in life, but also has direct costs to the economy.”
Previous research in this field has suggested a two-way relationship between loneliness and social standing. By using data collected over time, this research showed that feeling lonely negatively influenced a person’s social standing down the line, but social standing did not affect their future loneliness.
“Our research is one of very few studies reporting on the impact of loneliness years later. If we are to create effective prevention strategies, we need to continue collecting data in order to unravel the long-term outcomes of loneliness at various stages of life.
“We need more longitudinal data to unravel the long-term outcomes of loneliness at various stages of life. This can offer insight for developing prevention strategies.”
The study’s researchers argue that their findings highlight the importance of effectively tackling loneliness in order to help both the individual and society.
“While we should never forget that loneliness impacts people of all ages, our research suggests that reducing loneliness in children and young people could yield benefits both for their own employment prospects and for the economy more widely.”
This study was possible thanks to funding from the Colt Foundation and the Medical Research Council, with additional support from the National Institute of Child Health and Human Development and by the Jacobs Foundation.
The socioeconomic consequences of loneliness: evidence from a nationally representative longitudinal study of young adults (DOI 10.1016/j.socscimed.2024.116697) (Bridget T. Bryan, Katherine N. Thompson, Sidra Goldman-Mellor, Terrie E. Moffitt, Candice Odgers, Sincere Long Shin Soa, Momtahena Uddin Rahman, Jasmin Wertz, Timothy Matthews, Louise Arseneault) was published in Social Science and Medicine.
For more information, please contact Patrick O’Brien (Media Manager, King’s IoPPN)
Categories
Follow Us
For the latest updates and news, follow us on our social channels.












Recent Comments